Year: 2019 Title: CAROLINA TRIAL Subtitle: Effect of Linagliptin vs Glimepiride on Major Adverse Cardiovascular Outcomes in Patients With Type 2 Diabetes Type of Trial: An International, Randomised, Parallel Group, Double Blind Trial Objective: To assess cardiovascular outcomes of linagliptin … Read More
diabetes


AiDAPT Trial: Automated Insulin Delivery in Pregnancy Complicated by T1DM
Year: 2023 Title: AiDAPT TRIAL Subtitle: Automated Insulin Delivery in Women with Pregnancy Complicated by Type 1 Diabetes Type of Trial: Interventional, randomized controlled trial Objective: To find definitive proof of a benefit to women by using automated closed-loop for … Read More
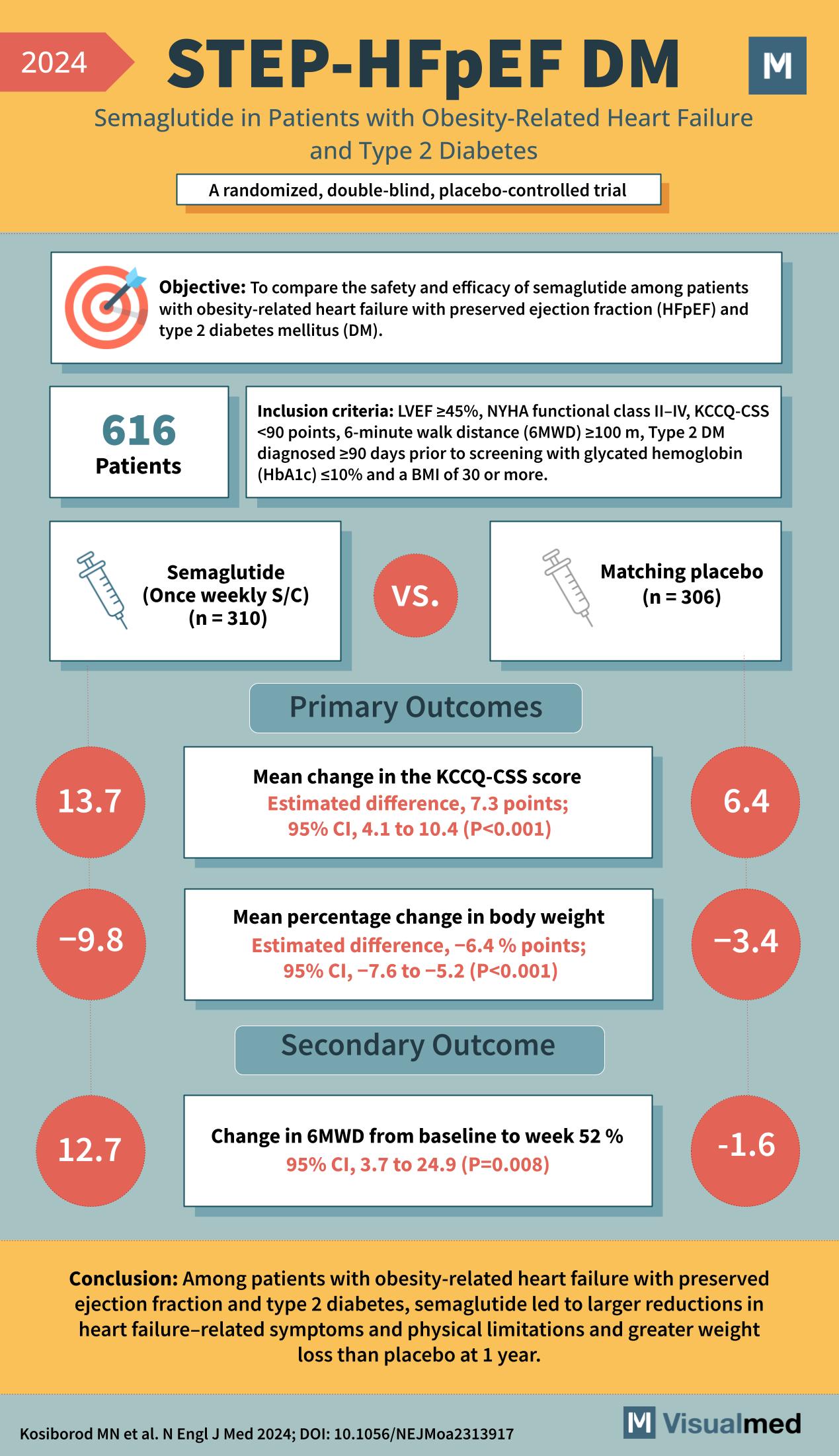
STEP-HFpEF DM: Semaglutide in HFpEF and DM
The study suggests that Semaglutide is effective in reducing symptoms and weight in patients with obesity-related heart failure with preserved ejection fraction and type 2 diabetes when compared to a placebo

DAPA-MI Trial: Dapagliflozin in MI
DAPA-MI Trial: Dapagliflozin in MI? The DAPA-MI Trial, as reported in the New England Journal of Medicine in 2023, was a randomized, double-blind clinical trial designed to assess the safety and efficacy of dapagliflozin, a medication typically used to treat … Read More
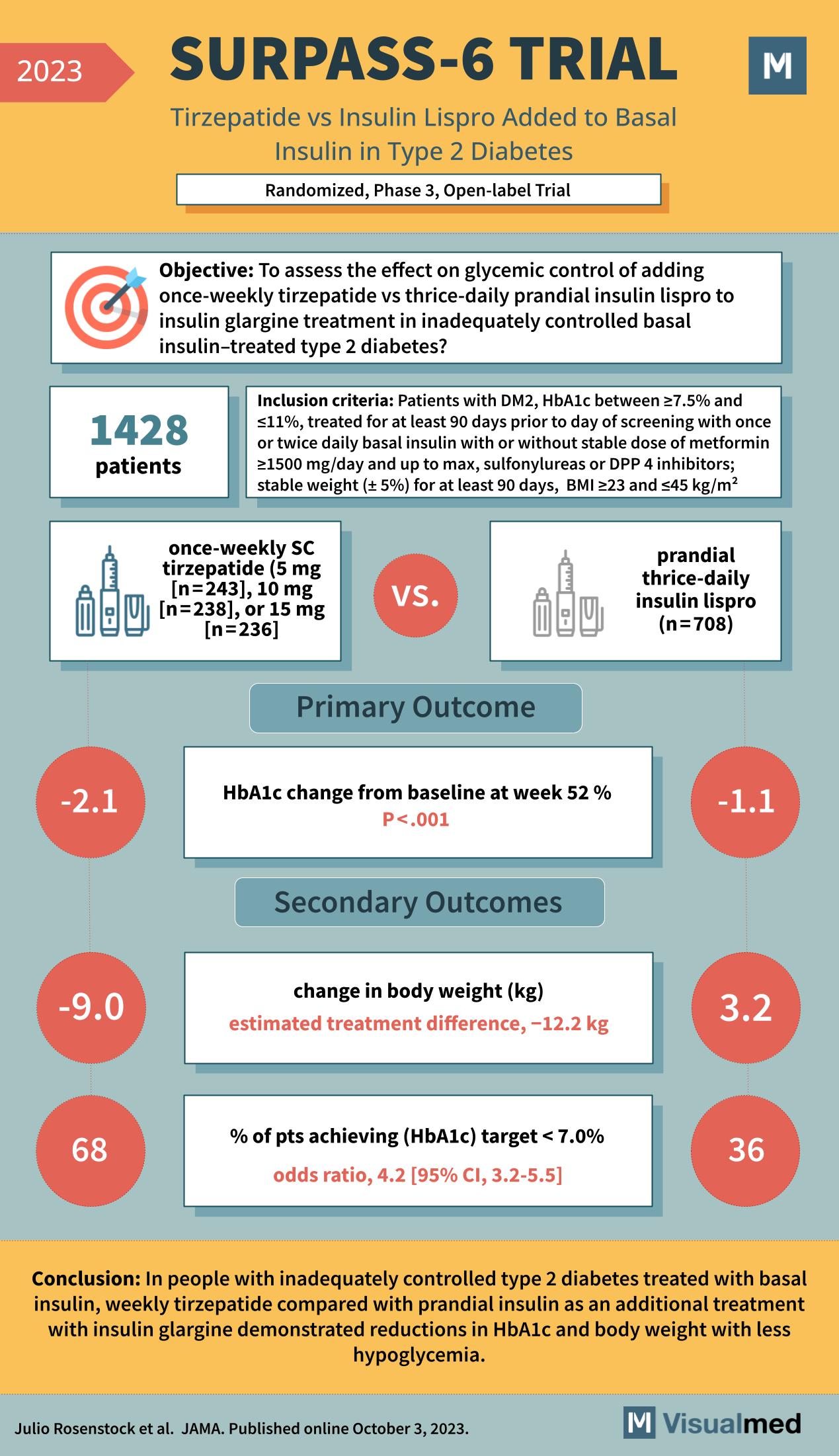
SURPASS-6 Trial: Tirzepatide in T2DM
The SURPASS-6 trial, featured in JAMA in October 2023, represents a significant advancement in the treatment of type 2 diabetes. This randomized, phase 3, open-label trial was designed to evaluate the effects of once-weekly subcutaneous (SC) tirzepatide versus thrice-daily prandial … Read More

SELECT Trial: Semaglutide and CV outcomes
Semaglutide Improve CV events? SELECT Trial Summary The SELECT trial, a pivotal study published in the New England Journal of Medicine (NEJM) in November 2023, has offered the medical community valuable insights into the treatment of cardiovascular (CV) events in … Read More

ADVANCE Trial Summary: Intensive Glucose Control in Diabetes Type 2
2008 ADVANCE TRIAL Intensive Blood Glucose Control and Vascular Outcomes in Patients with Type 2 Diabetes Multicenter, factorial, randomized trial Objective: To evaluate vascular effects of intensive glycemic therapy targeting a HbA1c <6.5% in patients with type II diabetes 11,140 … Read More
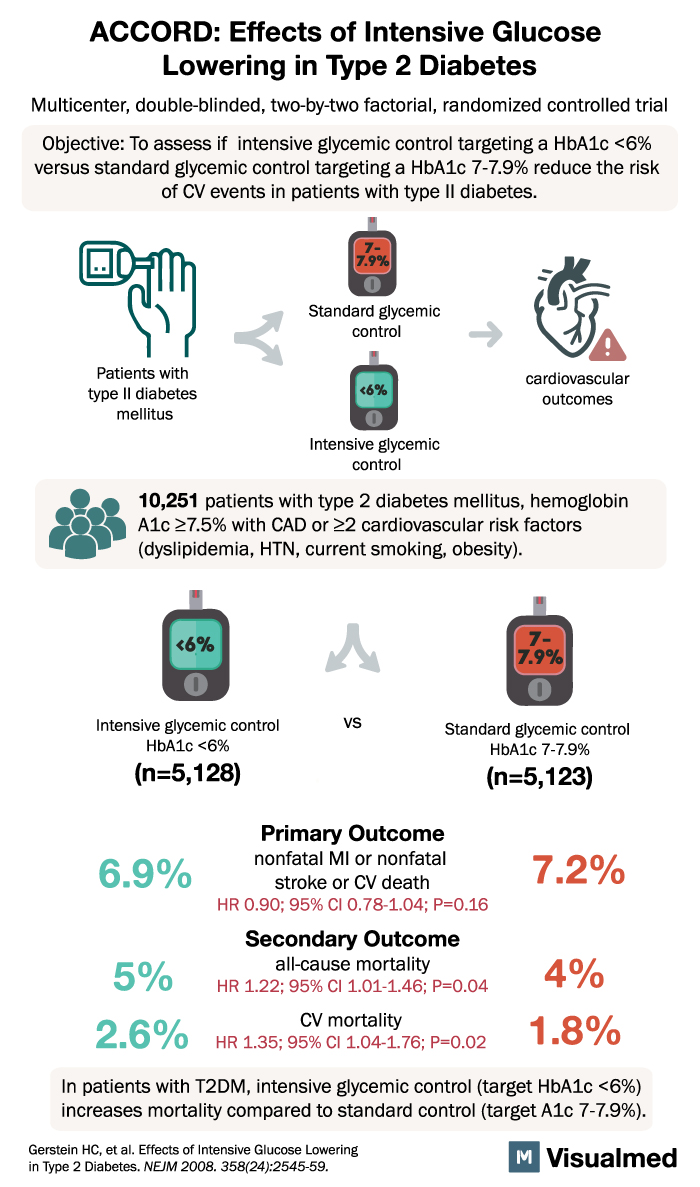
ACCORD Trial: Intensive Glucose Lowering in DM2
ACCORD: Effects of Intensive Glucose Lowering in Type 2 Diabetes Multicenter, double-blinded, two-by-two factorial, randomized controlled trial Objective: To assess if intensive glycemic control targeting a HbA1c <6% versus standard glycemic control targeting a HbA1c 7-7.9% reduce the risk of … Read More

ACCORD BP Trial Summary: Intensive BP Control in Type 2 Diabetes
2010 ACCORD BP TRIAL Effects of intensive blood-pressure control in type 2 diabetes mellitus Multicenter, randomized, controlled, open-label trial Objective: In patients with T2DM at high risk for CV events, does intensive BP control (SBP <120 mmHg) reduce rates of … Read More