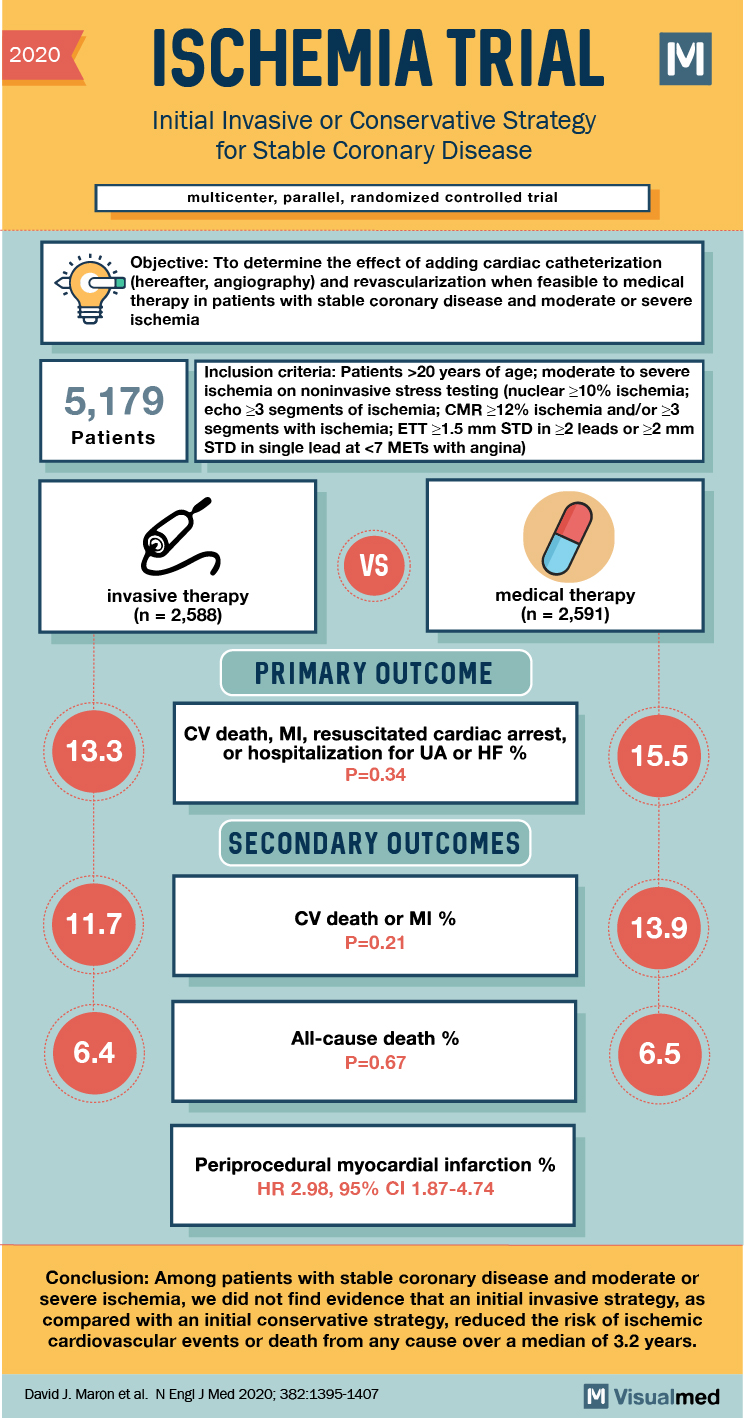
2020 ISCHEMIA TRIAL M Initial Invasive or Conservative Strategy for Stable Coronary Disease multicenter, parallel, randomized controlled trial Objective: Tto determine the effect of adding cardiac catheterization (hereafter, angiography) and revascularization when feasible to medical therapy in patients with stable … Read More
CAD

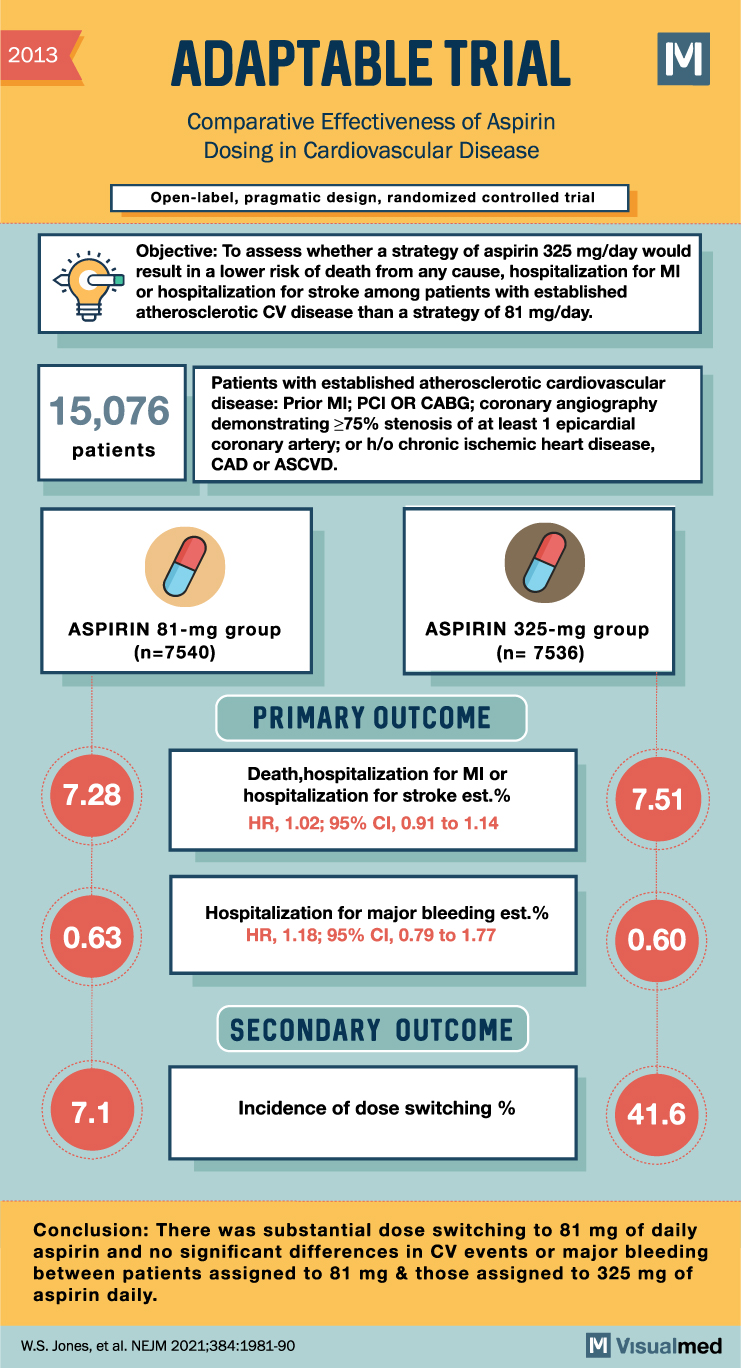
ADAPTABLE Trial Summary: Aspirin Dosing in CV Disease
2013 ADAPTABLE TRIAL Comparative Effectiveness of Aspirin Dosing in Cardiovascular Disease Open-label, pragmatic design, randomized controlled trial M Objective: To assess whether a strategy of aspirin 325 mg/day would result in a lower risk of death from any cause, hospitalization … Read More
Tags: aspirin, CAD, coronary artery disease

POPULAR CABG Trial Summary: Ticagrelor in CABG
2020 POPULAR CABG TRIAL Effect of adding ticagrelor to standard aspirin on saphenous vein graft (SVG) patency in patients undergoing coronary artery bypass grafting double-blind, placebo-controlled, multicenter, randomized controlled trial M Objective: To assess whether ticagrelor added to standard aspirin … Read More
Tags: CABG, CAD, coronary artery disease, graft, SVG, ticagrelor